35,000+ smart investors are already getting financial news, market signals, and macro shifts in the economy that could impact their money next with our FREE weekly newsletter. Get ahead of what the crowd finds out too late. Click Here to Subscribe for FREE.
Canada’s health-care system has long been tied to national pride and shared identity. For decades, it symbolized access without fear of bills. That confidence is starting to fray. Across provinces, warning signs are becoming harder to ignore. Patients wait longer. Workers leave faster. Costs climb while outcomes stall. Rural areas feel the strain first, but cities are catching up. Here are 20 signs Canada’s health-care system is reaching a breaking point.
Emergency Room Wait Times Keep Stretching Longer
20 Signs Canada’s Health-Care System Is Reaching a Breaking Point
- Emergency Room Wait Times Keep Stretching Longer
- Family Doctor Shortages Are Spreading Beyond Rural Areas
- Health-Care Workers Are Leaving Faster Than They Are Replaced
- Surgical Backlogs Keep Growing Despite Recovery Plans
- Ambulance Offload Delays Are Becoming Normalized
- Hospital Beds Are Occupied by Patients with Nowhere Else to Go
- Long-term Care Capacity Falls Short of Demand
- Mental Health Services Remain Hard to Access
- Rural Communities Face Shrinking Health Access
- Diagnostic Test Waits Delay Treatment Decisions
- Health-Care Spending Rises Without Matching Outcomes
- Data Sharing Between Provinces Remains Limited
- Preventive Care Gets Crowded Out by Crisis Care
- Health Inequities Are Becoming More Visible
- Medical Training Bottlenecks Limit Future Supply
- Public Trust Shows Signs of Strain
- Technology Adoption Moves Slower Than Expected
- Public Health Capacity Remains Stretched Thin
- Policy Changes Take Years to Show Results
- Canadians Are Turning to Private Options Out of Necessity
- 22 Groceries to Grab Now—Before another Price Shock Hits Canada

Emergency rooms are meant for urgent care, yet many Canadians wait hours before seeing a doctor. Some waits stretch past eight hours. Others last an entire day. Hallway medicine has become routine in several hospitals. Patients sit on chairs or stretchers without privacy. Staff rush between cases with little downtime. Triage systems struggle under volume pressure. Seasonal spikes no longer explain delays. Even calm periods feel overloaded. When emergency rooms clog, ambulances wait outside instead of responding to new calls. That bottleneck ripples through the entire system.
Family Doctor Shortages Are Spreading Beyond Rural Areas

Finding a family doctor used to be easier in cities. That advantage is fading. Many urban clinics stop accepting new patients. Retiring physicians outnumber replacements in some regions. Younger doctors often avoid traditional practices. Paperwork, long hours, and overhead costs deter them. Walk-in clinics fill gaps but lack continuity. Patients repeat histories at every visit. Preventive care suffers without long-term relationships. Chronic conditions go unmanaged until they worsen. The system becomes reactive instead of steady. A missing family doctor now affects millions of Canadians.
Health-Care Workers Are Leaving Faster Than They Are Replaced

Burnout has shifted from a concern to a constant reality. Nurses report exhaustion after years of overtime. Many leave bedside roles entirely. Others move abroad or into the private sector. Recruitment cannot keep pace with departures. Training pipelines take years to fill gaps. Temporary staff cost more and know less about local systems. Remaining workers shoulder heavier loads. Morale drops further. Errors become more likely under pressure. A system cannot function without people willing to stay. Right now, many are choosing not to.
Surgical Backlogs Keep Growing Despite Recovery Plans

Elective surgery backlogs surged during pandemic shutdowns. Recovery plans promised quick relief. Progress remains uneven. Some patients wait months for joint replacements. Others delay procedures that restore basic mobility. Pain management becomes the interim solution. That approach has limits. Delays worsen outcomes and recovery times. Surgeons face packed schedules with limited operating room hours. Staffing shortages slow throughput. Patients grow frustrated and anxious. Backlogs are no longer a short-term issue. They have become a standing feature.
Ambulance Offload Delays Are Becoming Normalized

Ambulances increasingly wait outside hospitals instead of returning to service. Crews sit with patients for hours. Emergency bays lack space. Stretched staff cannot accept new arrivals. While ambulances wait, response times rise elsewhere. Heart attacks and strokes lose critical minutes. Paramedics face stress without relief. Communities feel less protected. These delays once made headlines. Now they barely register. Normalizing this pattern hides serious risk. Emergency response systems depend on speed. Delays weaken that foundation.
Hospital Beds Are Occupied by Patients with Nowhere Else to Go
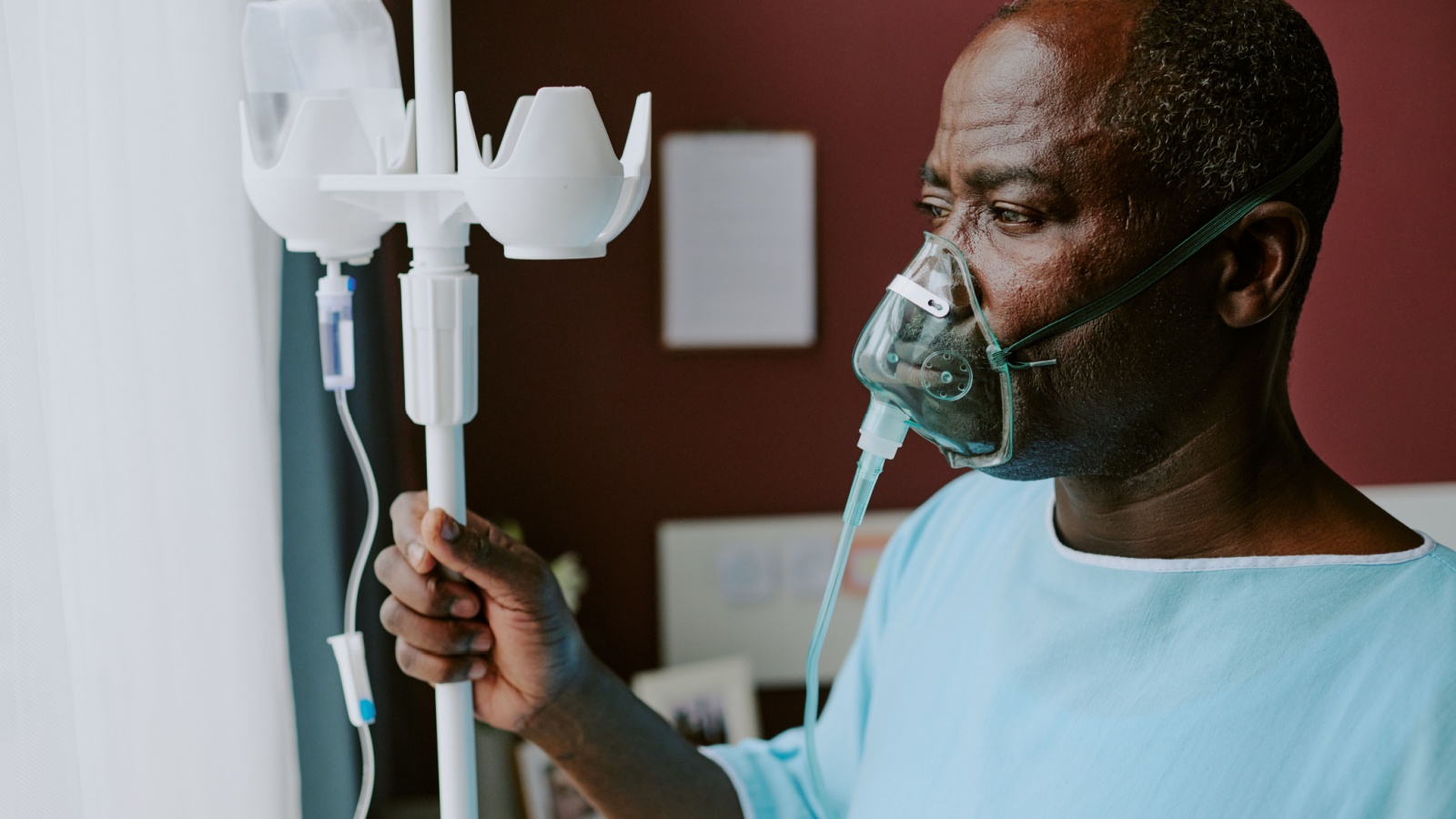
Many hospital beds are filled by patients ready for discharge. They remain due to missing home care or long-term care spaces. This phenomenon blocks acute care access. Emergency rooms back up as a result. Families struggle to arrange alternatives. Staff manage social needs alongside medical ones. Hospitals were not built for this role. The system becomes gridlocked. Solving bed shortages requires action beyond hospitals. Without that, flow problems persist and worsen.
Long-term Care Capacity Falls Short of Demand

Canada’s population is aging quickly. Long-term care capacity has not kept pace. Waitlists stretch for months or years. Families scramble to support aging relatives. Caregiver burnout rises quietly. Facilities face staffing gaps and rising costs. Quality varies widely between homes. Public trust was damaged during recent crises. Demand continues to grow regardless. Without sufficient spaces, hospitals absorb overflow. That pressure spreads system-wide and limits flexibility.
Mental Health Services Remain Hard to Access

Mental health needs have risen across age groups. Access has not matched demand. Publicly funded therapy often has long waits. Private care remains expensive. Emergency rooms handle mental health crises instead. That setting lacks continuity and privacy. Youth face especially limited options. Early intervention opportunities are missed. Conditions worsen before treatment begins. Mental health care remains fragmented. The system treats symptoms rather than stability. That imbalance strains patients and providers alike.
Rural Communities Face Shrinking Health Access
Rural communities across Canada are losing reliable access to care. Emergency rooms reduce hours or close overnight. Some towns rely on rotating doctors who stay briefly. Residents travel long distances for basic services. Winter weather adds risk and delay. Recruitment remains difficult despite financial incentives. Locals postpone care because trips are costly and time-consuming. Minor issues escalate into serious problems. Transfers to urban hospitals increase pressure elsewhere. Rural decline rarely makes headlines, yet it quietly reshapes outcomes.
Diagnostic Test Waits Delay Treatment Decisions

Diagnostic tests shape nearly every treatment plan. Many Canadians wait weeks for scans or specialist tests. Results arrive slowly, delaying next steps. Physicians hesitate without confirmation. Patients live with pain or uncertainty during the wait. Conditions progress while paperwork moves. Imaging backlogs vary by region, creating uneven access. Some turn to private clinics for speed. Public queues grow longer as a result. Diagnosis should clarify care. Instead, it often stalls momentum. Delayed testing increases anxiety, worsens outcomes, and strains already crowded clinics.
Health-Care Spending Rises Without Matching Outcomes

Canada spends more on health care each year. Outcomes do not rise at the same pace. Wait times remain long. Staffing shortages persist. Administrative layers absorb growing budgets. Frontline workers report limited relief. Patients struggle to see improvements despite higher costs. Money flows unevenly across provinces and programs. Public frustration builds when results feel unchanged. Spending alone cannot fix structural issues. Without reform, added funding produces diminishing returns. A system under strain needs smarter allocation, not just larger budgets that fail to reach patients directly.
Data Sharing Between Provinces Remains Limited

Health data rarely moves smoothly between provinces. Patients repeat histories at every visit. Tests get duplicated because records are unavailable. Transfers involve delays and confusion. Technology systems differ widely by region. Integration efforts move slowly. Providers lose time chasing information. Errors become more likely without full context. Patients shoulder the inconvenience. A modern health system depends on shared records. Fragmented data keeps care inefficient and costly. As mobility increases, this gap becomes harder to justify and more damaging to outcomes.
Preventive Care Gets Crowded Out by Crisis Care

Preventive care reduces long-term strain on health systems. Current pressures push it aside. Clinics prioritize urgent cases over screenings. Routine checkups get delayed or skipped. Lifestyle counseling receives less attention. Chronic conditions worsen quietly. Patients return later with advanced problems. Emergency departments absorb preventable cases. Prevention lacks urgency compared to crises. That imbalance fuels future demand. Without space for early care, the system stays reactive. Over time, neglected prevention multiplies costs, suffering, and hospital congestion.
Health Inequities Are Becoming More Visible

Health access varies sharply across communities. Income, location, and background shape outcomes. Marginalized groups face longer waits and fewer options. Language barriers complicate treatment. Indigenous communities report chronic shortages. Urban poverty limits follow-up care. Private alternatives widen gaps. Universal coverage promises fairness. Reality often falls short. Visible inequity signals system stress. When access depends on circumstance, trust erodes. A strained system exposes disparities that were once easier to overlook but now demand attention.
Medical Training Bottlenecks Limit Future Supply

Canada trains fewer doctors than the population requires. Medical school seats remain limited. Residency positions cap growth. International graduates face long licensing paths. Training takes years to translate into care. Planning cycles lag demographic change. Retirements outpace new entries. Shortages persist despite student interest. Workforce decisions today shape access decades later. Without expanding pathways, gaps widen. Delayed action guarantees future strain. A system nearing capacity cannot afford slow pipeline growth.
Public Trust Shows Signs of Strain

Canadians still value universal health care. Confidence feels less certain. Media stories highlight delays and failures. Personal experiences spread quickly online. Expectations clash with reality. Frustration grows when care feels inaccessible. Trust weakens when promises seem unmet. Rebuilding confidence requires visible improvement. Silence worsens doubt. A health system depends on public belief as much as funding. When trust erodes, patience fades. That shift signals deeper instability within the system.
Technology Adoption Moves Slower Than Expected

Digital tools promise efficiency and access. Progress remains uneven. Fax machines still dominate communication. Virtual care expanded but lacks integration. Patients juggle portals and logins. Staff manage multiple systems daily. Poor rollout creates friction instead of relief. Technology should reduce the workload. Instead, it often adds steps. Slow adoption wastes time and resources. A strained system cannot afford clunky tools. Delayed modernization compounds pressure across clinics, hospitals, and administrative teams.
Public Health Capacity Remains Stretched Thin

Public health teams manage prevention and surveillance. Staffing levels remain tight. Routine work competes with emergencies. Burnout affects inspectors and planners. Preparedness suffers without buffer capacity. Data collection slows under pressure. Community outreach declines. Prevention depends on steady resources. Thin margins leave little room for crises. When public health weakens, hospitals feel the impact later. Strain here often goes unnoticed until consequences emerge across the broader system.
Policy Changes Take Years to Show Results

Health policy moves slowly across jurisdictions. Political cycles interrupt continuity. Pilot programs stall before scaling. Frontline feedback often gets lost. Patients wait while plans evolve. Delayed results frustrate workers and users alike. Systems under stress need timely action. Long timelines deepen strain instead of easing it. Reform without speed feels distant. When improvement feels always years away, confidence drops. Slow policy response becomes another sign of a system stretched beyond comfort.
Canadians Are Turning to Private Options Out of Necessity

More Canadians seek private care to avoid long waits. Faster imaging and procedures attract those who can pay. This shift reflects frustration, not preference. Public queues grow longer as capacity shifts. Unequal access becomes visible. Universal principles feel diluted. Families face hard choices under pressure. When people bypass public care, it signals strain. A system meant to serve all loses cohesion. Rising private reliance marks a breaking point many Canadians never expected to face.
22 Groceries to Grab Now—Before another Price Shock Hits Canada

Food prices in Canada have been steadily climbing, and another spike could make your grocery bill feel like a mortgage payment. According to Statistics Canada, food inflation remains about 3.7% higher than last year, with essentials like bread, dairy, and fresh produce leading the surge. Some items are expected to rise even further due to transportation costs, droughts, and import tariffs. Here are 22 groceries to grab now before another price shock hits Canada.
22 Groceries to Grab Now—Before another Price Shock Hits Canada
This Options Discord Chat is The Real Deal
While the internet is scoured with trading chat rooms, many of which even charge upwards of thousands of dollars to join, this smaller options trading discord chatroom is the real deal and actually providing valuable trade setups, education, and community without the noise and spam of the larger more expensive rooms. With a incredibly low-cost monthly fee, Options Trading Club (click here to see their reviews) requires an application to join ensuring that every member is dedicated and serious about taking their trading to the next level. If you are looking for a change in your trading strategies, then click here to apply for a membership.

